

Invasive Prenatal Diagnosis is a highly effective genetic diagnostic procedure used to test the fetus for chromosome abnormalities or detectable monogenic disorders. This method involves obtaining fetal tissue by inserting invasive sampling instruments. Prenatal Diagnosis typically utilizes either amniotic fluid or a sample of chorionic villi from the placenta.

Invasive prenatal testing is typically recommended by healthcare providers in the following situations:
Invasive Prenatal Diagnosis is a comprehensive method that enables accurate and reliable analysis of chromosomes and disease-causing gene variations in the fetus. It helps identify numerical or structural abnormalities in the chromosomes and detect genetic variations that may lead to the development of a genetic condition. This information allows obstetricians to make informed pregnancy management decisions. In contrast, Non-Invasive Prenatal Testing is merely a screening tool that only assesses the risk level of genetic diseases in the fetus without providing a definitive diagnosis.
Next-Generation Sequencing (NGS) technology and Sanger sequencing are utilized to identify various chromosomal abnormalities and inherited genetic disorders.
Chromosomal analysis of amniotic fluid or chorionic villi samples detects aneuploidy, which involves extra or missing copies of chromosomes. This assessment is vital to rule out aneuploidy, a common cause of miscarriage and birth defects. It identifies conditions like Down syndrome (Trisomy 21), Edwards syndrome (Trisomy 18), and Patau syndrome (Trisomy 13). Gender identification allows for detecting sex chromosome disorders like Klinefelter's syndrome and Turner syndrome. The test also detects unbalanced chromosomal rearrangements based on parental history, determining the severity of the disorder.
Genetic testing can be done on amniotic fluid or chorionic villus samples (CVS) to identify mutations in a fetus, particularly if one or both parents have a known genetic mutation. This testing can diagnose various inherited disorders, such as Beta Thalassemia, Cystic fibrosis, Sickle cell anemia, and Huntington Disease. Additionally, if requested, the sample can be tested for both chromosomal abnormalities caused by aneuploidy and inherited diseases.
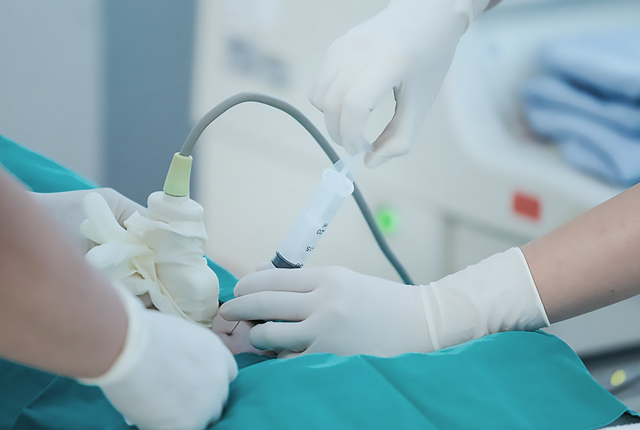
CVS and amniocentesis are ultrasound-guided procedures. There is a slight risk of miscarriage associated with both types of tests. It is advisable to discuss the implications of testing with your obstetrician and your partner before taking any decision.
Sample type: Amniotic Fluid
Description: Water-like substance surrounding the fetus in the amniotic sac, and which contains fetal cells
Sample collection: Done from 15 weeks onwards
Benefits: Provides a later diagnosis
Indication: Chromosomal aneuploidy screening to rule out confined placental mosaicism (prenatal condition of tissue-specific mosaicism in which a cytogenetic abnormality is confined to the placenta and is absent in the fetus)
Sample type: Chorionic Villi
Description: Tiny projections of placental tissue that contain the same genetic material as the fetus
Sample Collection: Done between 11-14 weeks of pregnancy
Benefits: Provides earlier diagnosis compared to other methods

An invasive prenatal test report will include results from 24-chromosome aneuploidy testing and/or genetic testing for monogenic disorders. The report will state if the tested fetus is affected by a chromosomal abnormality due to aneuploidy and/or genetic disease, based on the prescribed test. A euploid test result indicates that the fetus is less likely to have a chromosomal abnormality or an inherited condition, but not all genetic conditions can be ruled out.
There is a chance that the sample collected during amniocentesis/CVS procedures will be of maternal origin and not from the fetus - this is known as maternal cell contamination. To overcome this, a maternal blood sample should be collected separately to rule out contamination.

First Genomix offers counseling services to couples who receive test results indicating that their baby has a genetic or chromosomal condition. Our experienced counselors provide detailed discussions to help couples and their treating physicians carefully consider pregnancy management options.